We all know that exercise is a key component of a healthy lifestyle, but when it comes to conception and pregnancy, you might get completely different advice like “absolutely no exercise”, or “only gentle exercise”. It’s understandable that couples can feel confused or scared, and therefore decide it’s better to be safe than sorry. But we also know that exercise is a great way of maintaining overall fitness and reducing anxiety, so what should you do?
The quick answer is that everyone should keep their body moving in a safe and beneficial way, regardless of which stage of life you are in. You might think that this answer sounds vague, but the truth is that there is no one shape or form of exercise that suits everybody. Everyone’s body and preferences are different, and it’s really about finding an exercise routine that works best for your body.
Exercise and female fertility
The academic fields of sports nutrition, exercise physiology or lifestyle medicine are huge. Study after study has shown that regular exercise can effectively prevent chronic diseases such as cardiovascular disease, diabetes, certain types of cancers, and many more.
On the other hand, lack of exercise is closely linked to obesity, menstrual irregularities, ovulation dysfunction and poorer pregnancy outcomes.
In addition, it’s not just the overweight women who get affected. Studies have shown that even women with normal weight can experience lower fertility rates when living a sedentary lifestyle.
Having said that, too much vigorous exercise is also detrimental as competitive female athletes are more likely to have problems with their menstrual cycle, ovulation and fertility.
In a nutshell, too much or too little exercise are both bad for female fertility. Moderate and regular workouts are recommended for women of reproductive age.
Now the next question is: for women who are already diagnosed with sub- or infertility, could exercise make things a little better or worse?
One meta-analysis in 2019 compiled data from numerous studies to answer this question. The researchers concluded that regular exercise had beneficial effects on fertility and pregnancy outcomes as compared to no exercise while conceiving. In particular, the benefits were the most notable in patients with obesity, polycystic ovarian syndrome (PCOS), and insulin resistance.
Exercise and male fertility
What about for men? Considering that male infertility factors are equally important in conception planning, this is an important question to ask. Physical inactivity in men is also associated with reduced semen quality and lower sperm count. Interestingly, the hours spent on television watching is inversely associated with the sperm concentration and total sperm count.
Similar to the story with female athletes, strenuous exercise in men is also harmful, such as long periods of running and cycling. In fact, cycling is one the most troublesome forms of exercise for men due to the mechanical impact from sitting on the saddle, overheating the gonads, and wearing tight clothes. Research has convincingly shown abnormal sperm morphology and lower motility with men cycle for more than 5 hours a week. Another study showed that men who cycle just 1.5 hours of cycling per week had a substantially lower sperm concentration by 34%.
After examining several studies, the conclusion of a review study is that generally, sports should be beneficial or neutral for recreational athletes. However, professional athletes who engage in more strenuous sports are at risk for fertility problems. For most men, it is important to reduce scrotal heating, maintain a healthy weight, avoid smoking, alcohol, doping and environmental toxins during conception planning.
The impact of exercise on assisted reproductive technology (ART) outcomes
ART-powered conception and natural conception are quite different, and some practitioners would advice no exercise at all during IVF. This warning is mainly due to the rare but real risk of ovarian torsion, a condition in which the ovary twists and cuts its own blood supply. During ovarian stimulation, a step commonly involved in ART, ovaries are enlarged with more than usual developing follicles, which could increase the risk of ovarian torsion. Nonetheless, the risk is still extremely low, at about 0.03% of IVF cycles.
Confusingly, there is also evidence that one hour exercise three times per week improved implantation and pregnancy rates, while reducing the risk of miscarriage in a study of 436 women using intracytoplasmic sperm injection (ICSI) to conceive. Another study involving 131 women undergoing ART also showed that low to moderate exercise was associated with better live birth rates.
Considering both sides of the coin, some recommendations for women conceiving through ARTs are:
- Regular light to moderate exercises such as jogging, gentle yoga, light weights
- Avoid high impact exercises with quick twisting motions
- Avid quick changes in body position and inversions (such as in swimming and yoga)
- Avoid vigorous acrobatics
If you are still unsure about exercising in your unique medical condition, you could contact Melbourne-based fertility specialist, Dr. Alex Polyakov here.
Do consumer product chemicals affect fertility?
Environmental toxins are well-known risk factors for infertility, but every day, we are also exposed to many more non-persistent chemicals in consumer products. Do they also have an effect on people’s fertility and pregnancy outcomes?
The most probably chemicals to cause fertility problems are the endocrine-disrupting chemicals (EDCs). These are compounds that can affect hormonal pathways involved in the development of our reproductive systems and functions.
Endocrine disruptions may occur at multiple places in the body, including the hormonal control centre hypothalamus in the brain, the female ovaries, uterus and the male testis.
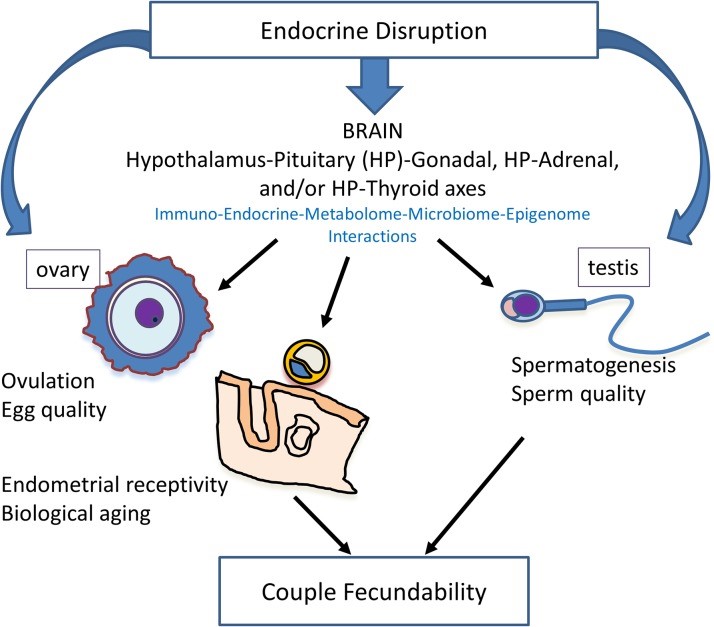
Human Reproduction Update, 2019
Among EDCs, you are probably most familiar with the names BPA and parabens. These are chemicals frequently found in consumer products such as plastics, personal care and cleaning products.
BPA (Bisphenol A)
BPA is a phenol used to produce plastics and is found in a variety of daily products, including water bottles, food cans, merchandise receipts and dental sealants. Oral ingestion is incredibly easy as BPA can leach into food and beverages from BPA-containing containers. Individuals who work with BPA-containing merchandise receipts are also susceptible to inhalation and skin absorption of BPA.
The half life of BPA is around 6 hours, meaning that it should not persist in the body for more than half a day. But during the short stay inside our bodies, BPA could potentially interact with a variety of hormone systems and affect reproductive function. Research has shown that BPA is a weak agonist of estrogen receptors and may interfere with estrogen signalling. In epidemiologic studies, urinary concentrations of BPA have been associated with higher risk of polycystic ovarian syndrome (PCOS) disrupted oocyte development, poorer semen quality, and IVF outcomes.
Parabens
Parabens are a group of chemicals that are used as preservatives in many household products. Their anti-bacterial and anti-fungal properties could conveniently increase the shelf life of many personal care products and food items. However, these chemicals also act as endocrine disrupters and can be absorbed through the skin, food, and air. Unfortunately, methyl paraben and ethyl paraben were detected in the urine of more than 90% of people! What’s more, paraben levels were reported to be 5-10 times higher in women than in men.
The effects of parabens have been studied in animals, which showed estrogenic, antiandrogenic, and thyroid activities. Although parabens do not accumulate in the human body, they have been detected in the breast and breast tumours. Moreover, epidemiological studies report associations of urinary parabens with lower semen quality, sex hormone dysfunctions, shortened menstrual cycles and lower antral follicle counts in women.
Phthalates
Phthalates are another class of chemicals used in numerous personal care products such as soap and cosmetics. They can also appear in pill capsules, food packaging and medical devices.
Phthalates have a half live of <24 hours and do not persist in the body. However, episodic exposures to phthalate are still associated with thyroid dysfunction, lower semen quality, altered sex hormones and lower oocyte yield, and increased risk of endometriosis. Phthalates may also decrease the implantation success in IVF cycles.
Takeaway
Exposure to potentially harmful chemicals in our daily lives is an unfortunate side effect to industrial advancement, which has also made our lives better in many other ways. What we can do is to continue learning about the unknown effects of such chemicals and try to minimise the exposure. As consumers, you may want to pay more attention to your personal care products to see if alarming chemicals are present in dangerous amounts.
